Bariatric patient's note
OUR GOAL IS TO GUIDE YOU THROUGH YOUR OPERATION IN THE SAFEST AND MOST EFFECTIVE WAY.
In addition to a well-performed surgery, we will use a number of globally proven measures to improve postoperative outcomes. These measures will begin before the operation and will continue after you return home.
CONSULTATION WITH A BARIATRIC SURGEON, ENDOCRINOLOGIST, PSYCHOLOGIST, DIETITIAN
First stage — the beginning of consultations with specialists of the multidisciplinary bariatric team. It may be conducted online or offline.
Second stage — it is necessary to undergo examination of the patient with obesity, namely:
- Complete blood count with differential.
- General urinalysis.
- Blood biochemistry: bilirubin, ALT, AST, creatinine, urea, total protein, albumin, C-reactive protein (CRP), creatine phosphokinase (CPK), lactate dehydrogenase (LDH).
- Coagulation profile: prothrombin index (PTI), bleeding time, prothrombin time (PT), thrombin time (TT), activated partial thromboplastin time (aPTT).
- Blood group.
- Wassermann reaction (RW).
- Markers of hepatitis B, C, HIV.
- Lipid profile: cholesterol, high-density lipoproteins (HDL), low-density lipoproteins (LDL), atherogenic index.
- Glycemic profile: blood glucose, insulin, glycated hemoglobin (HbA1c), HOMA index.
- Morning blood cortisol level or low-dose dexamethasone test: dexamethasone 1 mg (2 tablets) taken at 23:00, with blood sampling for cortisol at 08:00 the next morning.
- TSH, T3, T4 (free).
- hest X-ray. ECG, echocardiography, cardiologist consultation.
- Ultrasound of abdominal organs and lower limb vessels.
- Gastroduodenoscopy.
Third stage — a repeat consultation with specialists of the multidisciplinary bariatric team with a decision regarding the feasibility of bariatric surgery and preoperative preparation.
BEFORE SURGERY
WELL BEFORE SURGERY
Do not smoke. It has been shown that smoking worsens all postoperative outcomes, but especially increases the risk of infectious complications in the wound and abdominal cavity. Smoking cessation is an important step you can take to improve your health. Your surgical wound will heal faster and will be less likely to become infected if you stop smoking at least 4 weeks before surgery and for 8 weeks after surgery. The earlier you quit, the better for you.
Fitness (physical activity). Surgery always places stress on your body. However, if you are in good physical condition before surgery, this effect can be minimized. It is important to be as active and physically fit as possible before surgery. Physical exercise and a healthy diet will help you stay in shape. It is never too late to start adding activity to your daily routine. Exercises do not have to be intense. Try taking 15-minute walks 3 times a day and gradually increase your activity up to the day of surgery.
Avoid alcohol. Do not consume alcohol for 24 hours before surgery. Alcohol may cause an adverse reaction to medications you will receive in the hospital. Please inform us if you have ever experienced tremors or seizures after a period without alcohol.
Do not take narcotic or psychotropic drugs. If you use narcotic or psychotropic substances, discuss this privately with your surgeon. Any discussion about illegal drug use is confidential and will remain private. Our goal is your health and well-being. Since narcotic or psychotropic substances may cause dangerous complications during surgery, we need to know about all substances you are taking so that we can take the best possible care of you.
Plan ahead
Before surgery, we recommend that you arrange for help from family and friends when you return home. Each person recovers from surgery differently. It is difficult to predict what kind of help you will need. As a rule, we recommend that patients follow a light schedule for 1 month after surgery. When you go home, you should be able to perform light tasks such as climbing stairs, bathing, and eating. Just in case, make a plan with your loved ones to receive the necessary help:
- with meal preparation and stocking the refrigerator and freezer with foods that are easy to reheat;
- with bathing and personal care as needed;
- with household tasks such as cleaning and laundry;
- with caring for children or pets;
- with transportation to your appointments.
Start gathering information about those who can help you during your recovery.
Cancellation of surgery
If you become ill or pregnant, or for other reasons, call your surgeon as soon as possible and inform them.
DAY BEFORE SURGERY
1. What to bring with you for your hospital stay
Pack the following items to bring to the hospital:
- this brochure;
- a photo ID (ID card or passport);
- a list of substances you are allergic to;
- a list of all your current medications (prescription, over-the-counter, and herbal);
- recent test results;
- a robe, slippers or walking shoes, and pajamas;
- a toothbrush, toothpaste, soap;
- a bottle of still water, a cup, a spoon, a plate;
- 1 pack of your favorite sugar-free chewing gum;
- glasses, contact lenses, hearing aids, dentures, and containers for their storage labeled with your name (if needed);
- a cane, crutches, or a walker labeled with your name (if needed);
- all your CPAP equipment (mask and device), if you have sleep apnea;
- a magazine, book, or other reading materials if desired;
- loose and comfortable clothes for going home after discharge.
Bring only essential items. Please leave all valuables (jewelry, credit cards, money) at home. This includes piercing jewelry and tongue studs. You cannot wear any jewelry during surgery.
2. Hospital room
A surgical assistant will help you complete your inpatient medical record. After that, a nurse will escort you to your room and ask you to change into hospital clothing. You will meet your anesthesiologist (the doctor responsible for your sleep during surgery) and other members of your surgical team, who will answer any questions and ask you to sign consent forms.
3. Preoperative washing
It is important to follow the preoperative washing instructions to prevent infections. You will take 2 showers using a 0.05% chlorhexidine solution prescribed by your surgeon. Use 1 full bottle (200 ml) of 0.05% chlorhexidine for each shower.
The day before surgery:
- Take a shower before bedtime using 1 full bottle (200 ml) of 0.05% chlorhexidine as follows:
Step 1: Wash your face and hair with regular soap and shampoo and rinse completely.
Step 2: Use chlorhexidine solution to clean your body from the neck down, including the navel and up to the groin folds.
Step 3: Allow the chlorhexidine to be absorbed into the skin without rinsing it off.
- Do not use chlorhexidine to wash your hair.
- Do not shave the abdominal area where the surgery will be performed.
- Do not apply body lotions or hair conditioners after the shower.
- Wear clean clothes before going to bed.
Morning of surgery:
- Take a shower using 1 full bottle (200 ml) of 0.05% chlorhexidine.
- Do not use lotion, perfume, cosmetics, nail polish, jewelry, or piercings.
- Do not shave the abdominal area where the surgery will be performed.
- Put on clean clothes
It is very important to follow these instructions to prevent infection.
4. Preparation of the stomach and intestines
The day before surgery: follow a liquid or pureed diet throughout the entire day until midnight.
a. A liquid diet includes, for example:
- non-alcoholic beverages (ginger ale, cola, Sprite®);
- strained fruit juices without pulp (apple, white grape, orange, lemonade);
- water, tea, or coffee;
- kefir;
- chicken or beef broth;
- hard candies;
- fruit ice pops.
b. No solid food, only pureed products, for example blended lean chicken meat or fish such as hake.
c. Continue taking medications according to your doctor’s instructions.
DAY OF YOUR SURGERY
Food and drink on the morning of surgery:
- You may continue a clear liquid diet no later than 10 hours before the scheduled start time of the surgery.
- Stop drinking water 4 hours before surgery.
- Do not eat solid food.
- Take your medications with a sip of water approximately 2 hours before surgery.
- After this time, do not eat, drink, or put anything in your mouth. Do not use chewing gum or cough drops.
Preoperative area
A surgical assistant together with a nurse will help escort you to the preoperative room in the operating unit. Before the surgery, an intravenous catheter (into a vein) will be placed in your hand or forearm so that you can receive fluids and medications during the operation. You will again meet your anesthesiologist and other members of your surgical team who will be involved in the operation.
DURING SURGERY
You will be asleep and under the supervision of the medical team during the operation.
Family representative
It is helpful to appoint a family representative who can inform family members and friends about your condition after surgery. We cannot provide any medical information about you over the phone to unauthorized callers.
Waiting area
Relatives or friends may wait for you in the surgical department waiting area. Your family members may visit you as soon as you are in your hospital room. Your surgeon may wish to speak with your family or friends in a separate room after the operation, but this does not mean that anything went wrong during surgery. Your surgeon will also speak with you after the operation, but if you have not yet recovered from anesthesia, you may not remember this later.
AFTER SURGERY
Postoperative room
After surgery, you may wake up in the recovery room or in a hospital room — this is decided by the anesthesiologist. A nurse will monitor your blood pressure and pulse. The nurse will ask you about pain and make sure you are comfortable. You will stay here for several hours until you are fully awake.
You may have:
- an oxygen mask on your face;
- an intravenous catheter for administering fluids and medications;
- a urinary catheter (tube) that drains urine from the bladder.
When you are ready, you will be transferred to a hospital room. If the anesthesiologist determines that you are ready to be in the room immediately, you will be transferred under the supervision of a nurse to a hospital room.
Recovery in the hospital after surgery
You are the most important person on your recovery team. Walking, deep breathing, coughing, turning, and chewing gum are some of the things you can do to help yourself. The goals of the enhanced recovery program are:
- accelerated recovery;
- improved circulation;
- promotion of healing;
- improved bowel function;
- prevention of complications.
Your medical team will include:
- your surgeon (or “attending” surgeon);
- surgical department physicians;
- residents (surgeons in training);
- nurses;
- other specialists as needed, such as psychologists, dietitians, and physiotherapists.
While the attending surgeon is like the captain of the ship, the surgical staff and trainees work very closely as one team and are important “eyes and ears” in your care.
Goals for the evening after surgery:
- Pain management.
We will work with you to help control discomfort after surgery. When your pain is under control, you will be able to recover faster. Although no medication completely eliminates all pain, our goal is to manage the pain and ensure your comfort during recovery. The nurse will ask you to describe your pain using a scale from 0 (no pain) to 10 (the worst pain you can imagine). We want your pain to be below 4 (out of 10).
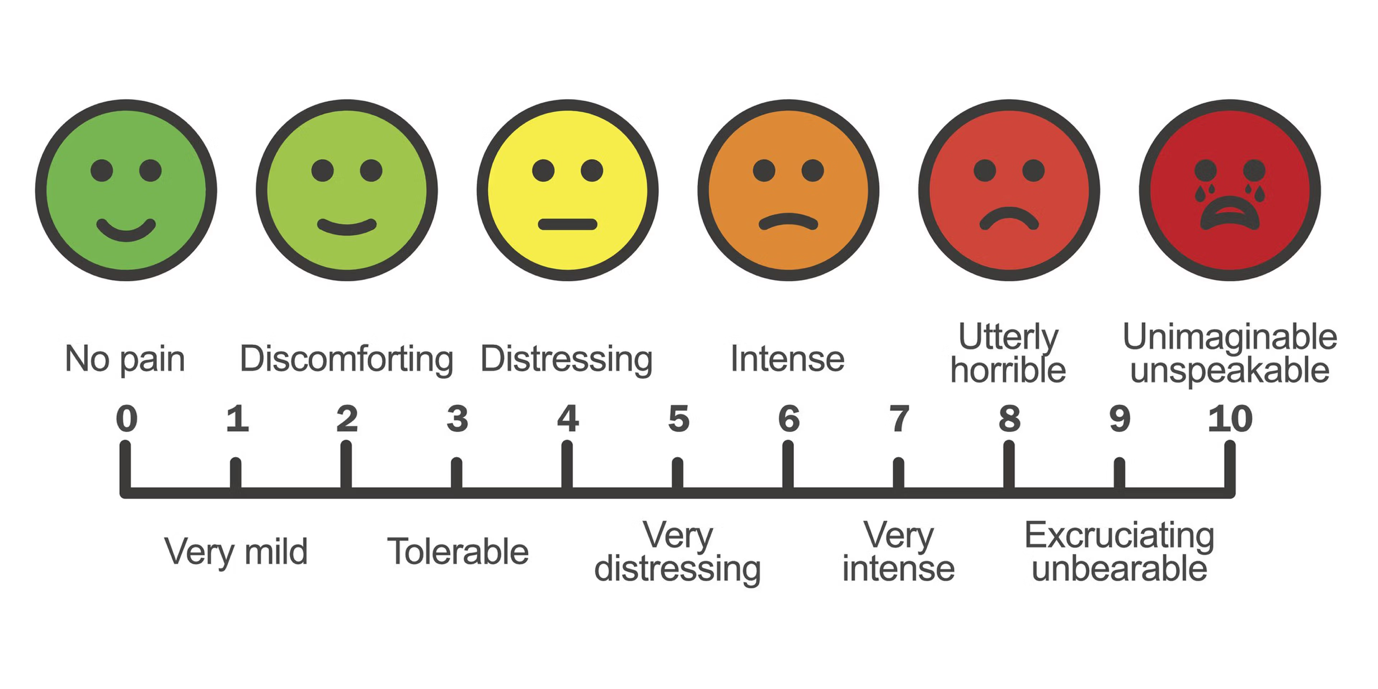
You will receive medications through an IV drip and orally to control pain discomfort. Some medications will be given continuously; others will be given as needed. Please let us know if your pain is not adequately controlled, and we will help you.
- Take deep breaths to prevent lung problems
- Get out of bed 2–3 hours after the end of surgery
- Drink fluids — still water up to 200 ml.
Goals for Day 1 (the first day after surgery):
1. Breathing
- Perform breathing exercises.
2. Activity
- Sit in a chair during meals.
- Take at least 4 walks in the corridor with assistance.
- Stay out of bed from time to time, for a total of up to 8 hours, as tolerated.
3. Pain control:
- Inform the nurse if your pain reaches 4 out of 10 on the pain scale.
4. Food and drink:
- Drink fluids to avoid dehydration — from 500 ml to 1 liter as recommended by your surgeon.
- Eat pureed food as tolerated.
- Chew gum for 30 minutes 3 times a day.
5. Drains and catheters:
- In most patients, the urinary catheter is removed on the first day if it was placed.
- In the morning, intravenous fluids will be discontinued and the IV catheter will be removed according to your surgeon’s recommendation, if there are no indications to continue infusions.
- Drains are removed on the first day, or your surgeon will inform you when they will be removed.
6. Thrombosis prevention:
- In addition to walking, you will receive an injection of an anticoagulant.
- You will be prescribed the oral medication rivaroxaban (Xarelto) for 30 days (as prescribed by your doctor).
When you can return home:
You will be ready to return home when you achieve the following goals:
- Your pain is controlled with oral medications only.
- You can walk without assistance.
- You can eat solid food (regular diet) without significant nausea.
- You do not have other problems that prevent you from returning home.
On the day of discharge, plan to return home by 2:00 PM. Before leaving, your doctor will review the discharge instructions with you. You will receive recommendations for medications that you will need to take at home. Before discharge from the hospital, we will provide you with information about your follow-up visit with the surgeon. If you have sutures that need to be removed, we will schedule an appointment for this 8–12 days after surgery.
Recovery at home after surgery
The condition of most patients improves with each day after surgery. Full recovery after surgery may take up to 1 month, but most patients experience rapid improvement within the first few days. Gradually, you will feel stronger and become more active. Follow the discharge instructions to support your recovery.
After surgery, unpleasant sensations are common. You may experience discomfort at the incision site and muscle pain. Getting up and moving can help relieve discomfort. Support the incision with a pillow when you cough or sneeze.
Your doctor will prescribe pain medication. Take it as directed. Some medications may negatively affect your stomach when taken on an empty stomach. To prevent nausea, take medication with food.
Call your doctor if you have any side effects such as:
- repeated vomiting;
- weakness up to loss of consciousness;
- dizziness;
- fever, body temperature above 38°C. Pain medications may cause constipation. To keep your bowel movements regular:
- drink more fluids;
- eat more whole grains, fruits, and vegetables;
- exercise regularly (a 15-minute walk is a good start);
- take stool softeners if your doctor advises you to do so.
Some of your pain medications may contain acetaminophen. Acetaminophen can cause liver damage if you take too much. Be sure to read labels carefully and follow your doctor’s instructions regarding medications. If you take Tylenol® (acetaminophen) for pain, do not take more than 3000 mg within 24 hours. If you are taking narcotic pain medications or sleeping pills, do not drink alcohol. You should not drive while taking narcotic pain medications.
Wound care
It is important that wounds remain clean and dry to prevent infection. This will help your wounds heal. Wash your hands before and after touching the wounds.
Daily wound care: continue to treat the wounds for 1 week with chlorhexidine once a day.
Do not apply lotions, creams, or ointments to the wounds unless prescribed by your doctor. You should wear comfortable clothing. Do not wear dirty or tight clothing over the wounds.
If you have paper tape strips (Steri-Strips™) on the skin over the incisions, leave them in place until they fall off. They provide additional support as the wound heals. No other dressing is required.
There are sutures that dissolve in the body and do not need to be removed. Bruising around the wound is common.
Inform your doctor about these signs of infection:
- significant redness, swelling, or pain in the area;
- thick discharge or pus from the wound.
Shower
You may shower 2 days after surgery. Let warm water run over the wounds and gently pat them dry. Do not rub. After that, treat the wounds with chlorhexidine and allow them to dry. Do not take a bath for 2 weeks.
Diet
Your appetite will not be normal immediately after surgery, but it should return within a few weeks. After surgery, you should be able to eat frequently in small portions.
Healthy nutrition will help your body recover. We recommend that you:
- eat foods containing protein, such as meat, poultry, fish, and dairy products;
- eat more often and in small portions throughout the day;
- try high-protein, high-calorie shakes;
- for now, avoid foods that cause stomach upset or diarrhea. Introduce them one at a time when you feel better.
Call your doctor if:
- you cannot drink fluids or keep them down;
- you have not had a bowel movement for 3 days.
Activity
Continue walking several times a day and gradually increase your activity. Rest if you feel tired. Try to get enough sleep. Taking pain medication before bedtime may be helpful if you have difficulty finding a comfortable sleeping position.
Do not lift anything heavier than 5–10 kg for 6 weeks after surgery. Lifting creates strain on the incision. You may walk, shower, and climb stairs. Do not overexert yourself.
For 6 weeks after surgery, avoid strenuous physical activity (weight training, stair-climbing machines, elliptical trainers, yoga, Pilates, and treadmills). As a rule, pain is your guide when increasing physical activity after surgery.
Driving
Your doctor will tell you when you can resume driving. Do not drive after taking narcotic medications or sleeping pills.
Sexual activity
Many people have questions about resuming sexual activity after surgery. If you feel well and well-rested, sexual activity may be resumed. Avoid positions that strain the incision site.
Work
We recommend that you take 2–3 weeks off after surgery. Patients with non- physical jobs may return to work when they feel well enough, which may occur as early as 1 week after surgery. However, it is difficult to predict energy levels after surgery. Patients whose work involves heavy physical labor may need a longer time off. Please discuss with your doctor when you can return to work.
When to call your doctor
Contact your doctor if you notice any of the following:
- body temperature above 38°C;
- discharge from the wound that may have an unpleasant odor;
- increased tension or tenderness of the wound;
- wound edges no longer meet;
- redness or swelling at the wound site;
- severe pain not controlled by your pain medications;
- nausea or vomiting that does not go away;
- inability to drink or retain fluids. If you cannot contact your doctor, go to the nearest emergency department.

